About Osteoporosis
Osteoporotic fractures
Osteoporosis is a bone disease affecting more than 200 Mio people in the world. In osteoporotic individuals, the density and quality of bones are reduced. This reduction occurs progressively and often there are no symptoms. As a result, bones become weak and the risk of fracture from a fall or, in serious cases, from minor trauma dramatically increases.
With progressive rise in life expectancy, osteoporosis is becoming a socio-economic challenge. These so-called fragility fractures decrease the quality and lifespan of affected patients. The associated social and economic costs represent a societal burden already today.

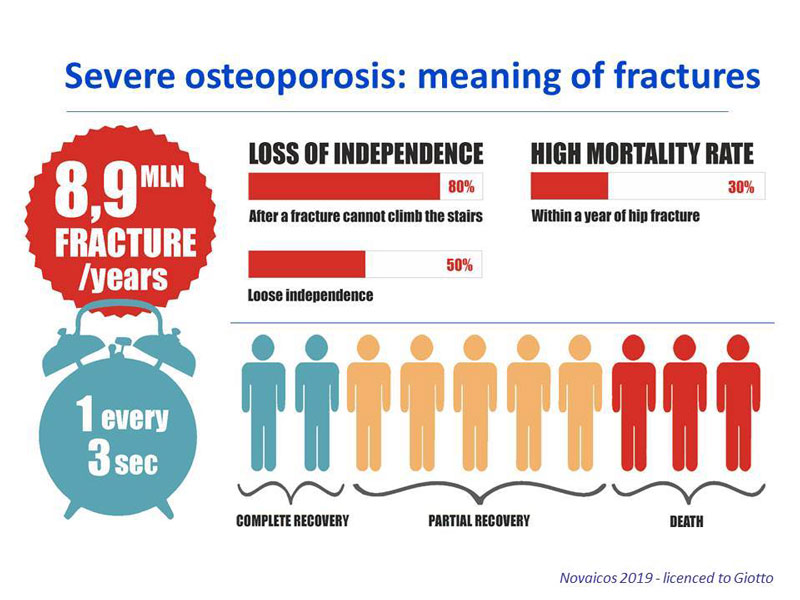
It has been estimated that globally, 1 in 3 women and 1 in 5 men aged fifty years and over will experience an osteoporotic fracture once in their life. Fragility fractures have been estimated to occur at the rate of one every 3 seconds. The most common fractures sites are the hip, spine and wrist. Femoral fractures are more severe, as patients suffering with femoral fractures have been shown to die within a year (15-25%) or lose their independency (50%).
Vertebral fracture are often underdiagnosed, the presence of a vertebral fracture doubles the risk of subsequent femoral fracture within a year. Multiple vertebral fractures impair patients’ quality of life, cause acute and chronic pain and increase mortality.
Prevention of osteoporotic fractures
The prevention of osteoporosis relies mostly on educating the population on the effect of some factors that substantially increase the risk of incurring in a fragility fracture. Among the most relevant we mention:
– alcohol abuse
– smoking
– low calcium intake
– low body weight
– sedentary life
– usage of drugs with negative bone effect ( in e.g.corticosteroids).
These factors directly alter the bone metabolism and, with time, interfere with the maintenance of the bone tissue quality and strength.
Treatment
Although there are valid pharmacological treatments for the reduction of the risk, osteoporotic fractures occur and their surgical treatment is very challenging at all body sites. Standards implants for traumatology show limitations in fixing osteoporotic bones. In fact, the quality of the bone surrounding the implants is often so compromised that the entire fixation fails apart at minimal loading. Severely compromised bones do not heal and non-self-sufficient aged patients are prone to develop potentially deadly complications and comorbidities.
There is thus an unmet medical need for implants capable of improving the properties of the bone tissue surrounding them and increasing the chance to bring the fractured bone back to its form and function.